Dr. Elena Vasquez watched the lab results with growing concern, her coffee growing cold as she scrolled through the data on her computer screen. After fifteen years studying infectious diseases, she’d seen plenty of alarming trends, but this one made her stomach drop.
“We’re losing ground faster than I expected,” she muttered to her research partner, pointing at the resistance patterns displayed across multiple bacterial samples. The ancient killer they’d been tracking wasn’t just surviving modern antibiotics—it was learning to thrive despite them.
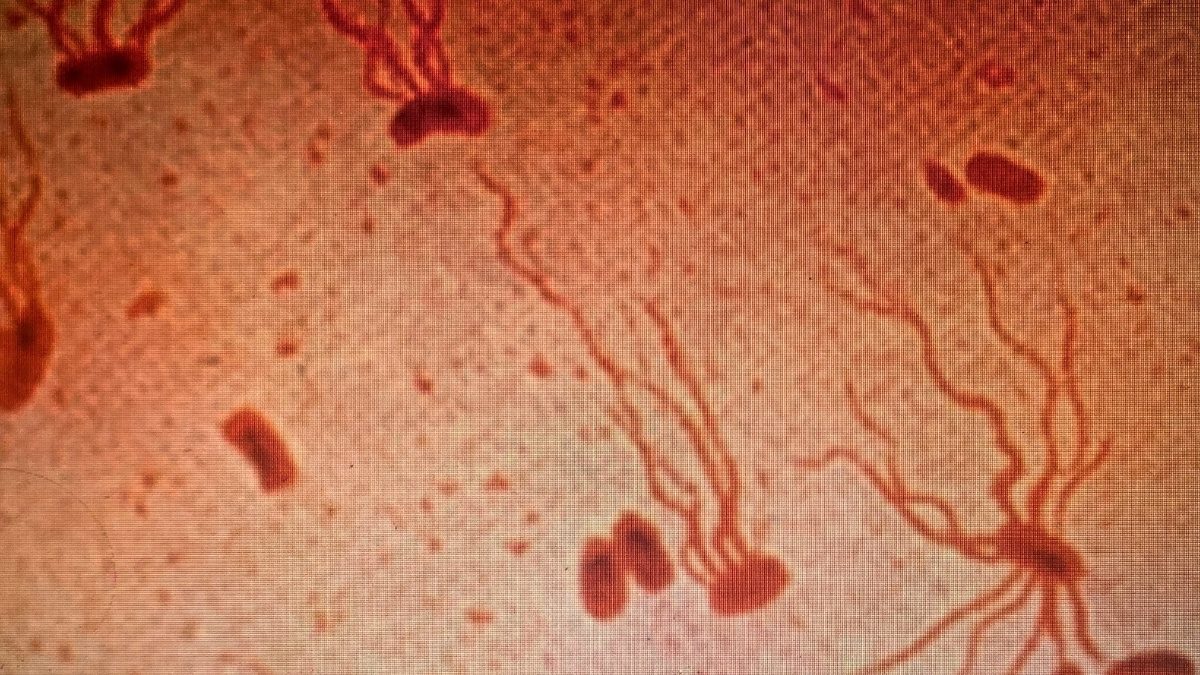
What Dr. Vasquez was witnessing in real-time represents one of the most urgent threats facing modern medicine today. Tuberculosis, the bacterial infection that has plagued humanity for thousands of years, is rapidly developing resistance to our most powerful antibiotics, and scientists are sounding the alarm louder than ever before.
The Ancient Enemy Gets Stronger
Tuberculosis isn’t some exotic disease from medical textbooks. It’s a living, breathing threat that infects roughly 10 million people worldwide each year, killing 1.6 million. What makes TB particularly dangerous isn’t just its deadly nature—it’s the bacterium’s remarkable ability to adapt and survive.
The latest research shows that drug-resistant tuberculosis cases are climbing at an alarming rate. Multidrug-resistant TB (MDR-TB) now accounts for nearly 500,000 new cases annually, while extensively drug-resistant TB (XDR-TB) continues to emerge in countries across the globe.
The speed at which TB is developing resistance is unprecedented. We’re seeing strains that laugh in the face of treatments that worked just five years ago.
— Dr. Marcus Chen, Infectious Disease Specialist
Unlike many modern diseases, tuberculosis has had millennia to perfect its survival strategies. Archaeological evidence shows TB infected humans as far back as 9,000 years ago, giving it plenty of time to develop sophisticated mechanisms for evading our immune systems and, now, our medications.
The bacterium spreads through airborne droplets when infected people cough, sneeze, or even talk. In crowded conditions with poor ventilation, a single person with active TB can infect dozens of others before symptoms even appear.
The Numbers Tell a Frightening Story
Recent data from the World Health Organization paints a stark picture of how rapidly antibiotic resistance is spreading. The statistics aren’t just numbers—they represent real people facing increasingly limited treatment options.
| Resistance Type | Annual Cases | Success Rate | Treatment Duration |
|---|---|---|---|
| Drug-Susceptible TB | 9.5 million | 85% | 6 months |
| Multidrug-Resistant TB | 500,000 | 60% | 18-24 months |
| Extensively Drug-Resistant TB | 25,000 | 34% | 24+ months |
The progression from treatable to nearly untreatable becomes clear when you look at these numbers. As resistance increases, treatment becomes longer, more expensive, and significantly less likely to succeed.
Several factors are accelerating this resistance development:
- Incomplete treatment courses when patients stop taking medications early
- Poor-quality antibiotics with inconsistent dosing
- Inadequate infection control in healthcare settings
- HIV co-infection, which weakens immune response
- Poverty and malnutrition that compromise treatment effectiveness
Every time someone doesn’t complete their full course of TB treatment, they’re essentially training the bacteria to become stronger. It’s like sending soldiers into battle but calling them back before they finish the job.
— Dr. Priya Sharma, Global Health Researcher
Who’s Really at Risk Right Now
While tuberculosis might seem like a distant concern for many Americans, the reality is more complex. Drug-resistant TB doesn’t respect borders, and global travel means resistant strains can appear anywhere within hours.
Certain populations face heightened risk. Healthcare workers treating TB patients encounter exposure regularly, especially in facilities with inadequate ventilation systems. People with compromised immune systems, including HIV patients and those undergoing cancer treatment, are particularly vulnerable.
Immigration patterns also play a role. Many drug-resistant TB cases in developed countries originate from regions where resistance is already widespread. This isn’t about blame—it’s about understanding how diseases spread in our interconnected world.
The economic impact extends far beyond healthcare costs. Families dealing with drug-resistant TB often face catastrophic expenses. Treatment can cost $100,000 or more per patient, and the extended treatment period means months or years of lost income.
We’re not just talking about a medical crisis—this is an economic disaster for families. I’ve seen people lose their homes trying to pay for TB treatment.
— Dr. Robert Kim, Public Health Economist
Children represent a particularly vulnerable population. Pediatric TB is often harder to diagnose, and drug-resistant strains in children typically indicate recent transmission from an adult with active disease.
What Scientists Are Doing to Fight Back
The medical community isn’t sitting idle while TB gains strength. Researchers are pursuing multiple strategies to stay ahead of this ancient killer.
New drug development has accelerated dramatically. For decades, TB treatment relied on the same handful of antibiotics developed in the 1940s and 1950s. Now, pharmaceutical companies and research institutions are testing novel compounds that attack the bacteria through different mechanisms.
Rapid diagnostic testing represents another crucial advancement. Traditional TB testing could take weeks to identify resistance patterns. New molecular tests can detect drug resistance within hours, allowing doctors to start appropriate treatment immediately rather than waiting for lab results.
Artificial intelligence is also joining the fight. Machine learning algorithms can analyze chest X-rays to identify TB cases faster than human radiologists, particularly important in resource-limited settings where specialist expertise may be scarce.
Technology is finally catching up to this ancient disease. We’re using 21st-century tools to fight a Stone Age killer, and that’s giving us hope we haven’t had before.
— Dr. Lisa Rodriguez, TB Research Consortium
Prevention strategies are evolving too. Better infection control in hospitals, improved contact tracing, and targeted screening in high-risk populations help identify cases before they spread.
The development of new vaccines also shows promise. While the current TB vaccine provides limited protection, several next-generation vaccines are in clinical trials, potentially offering better protection against both infection and disease progression.
The Race Against Time
Every month that passes without aggressive action makes the problem worse. Drug-resistant tuberculosis isn’t a future threat—it’s a current crisis that’s accelerating.
The good news is that we’re not helpless. Unlike some other disease outbreaks, we understand how TB spreads and what drives resistance. The challenge lies in implementing solutions quickly enough and broadly enough to make a difference.
Success requires coordination between governments, healthcare systems, researchers, and communities. No single intervention will solve the problem, but a comprehensive approach combining new drugs, better diagnostics, improved prevention, and sustained funding can turn the tide.
The stakes couldn’t be higher. If current trends continue, we could face a world where tuberculosis becomes essentially untreatable—a return to the pre-antibiotic era when a TB diagnosis was often a death sentence.
FAQs
Can drug-resistant tuberculosis spread to the United States?
Yes, it already has. The US reports several hundred cases of multidrug-resistant TB annually, mostly linked to international travel or immigration.
How long does treatment for drug-resistant TB take?
Treatment can last 18-24 months or longer, compared to 6 months for regular TB, and requires multiple daily medications with significant side effects.
Is there a vaccine for tuberculosis?
The BCG vaccine exists but provides limited protection. Several improved vaccines are currently in development and clinical trials.
What makes TB bacteria so good at developing resistance?
TB bacteria reproduce slowly and can remain dormant for years, giving them time to develop mutations that help them survive antibiotic treatment.
Can healthy people get drug-resistant tuberculosis?
Yes, though people with compromised immune systems face higher risk. However, anyone exposed to drug-resistant TB can become infected regardless of their overall health.
How expensive is drug-resistant TB treatment?
Treatment costs can exceed $100,000 per patient due to expensive medications, extended treatment duration, and frequent monitoring requirements.